What if the answer to preventing type 2 diabetes was hiding in your sleep schedule all along? A fresh study from researchers analyzing nearly 23,500 Americans has uncovered something surprisingly specific: approximately 7 hours, 19 minutes, and 12 seconds appears to be the sweet spot for protecting yourself against insulin resistance and the metabolic decline that often precedes diabetes.
The findings, published in BJM Open Diabetes Research Care, tracked participants' sleep patterns and compared them against their estimated glucose disposal rate (eGDR), a key indicator of how well the body processes insulin. Higher eGDR scores mean lower risk of insulin resistance. The results reveal something unexpected about sleep and health that most wellness advice gets wrong.
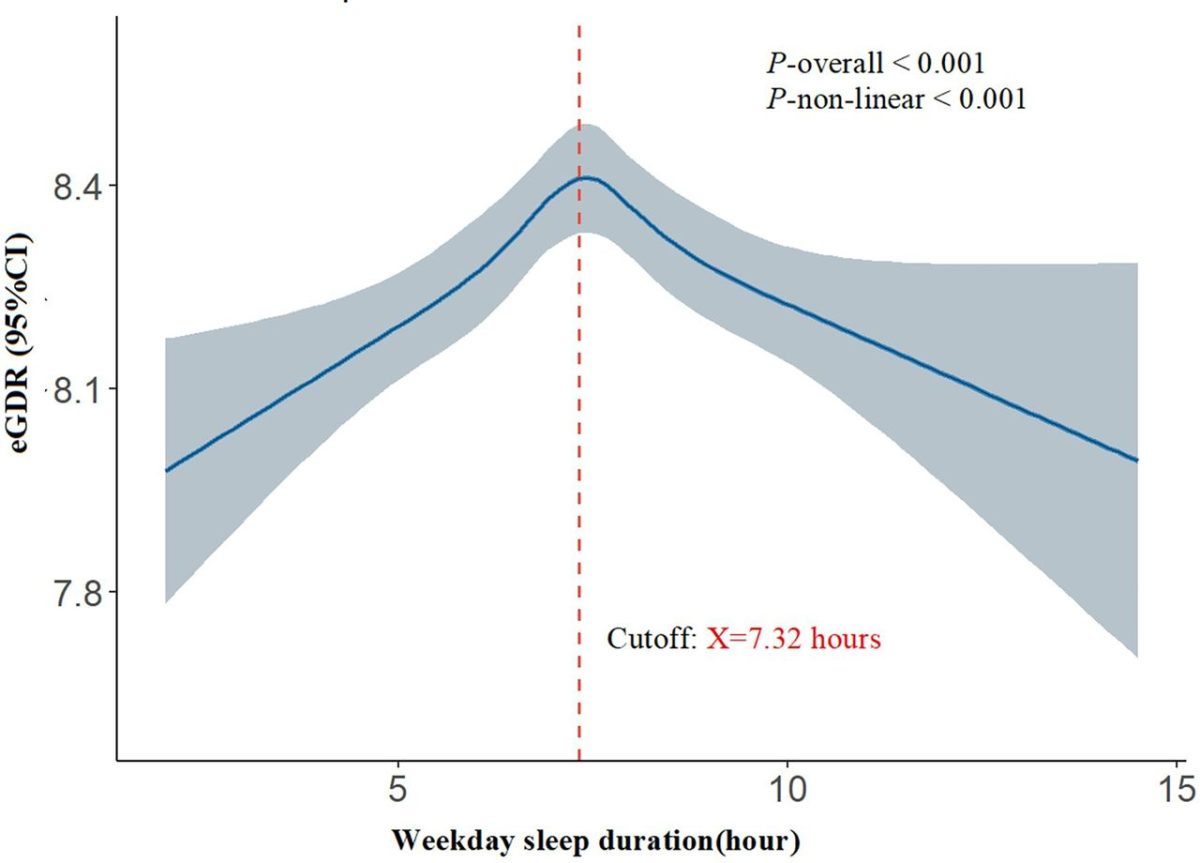
Why sleep duration matters more than you realize
Diabetes remains a staggering global health challenge. More than 40 million Americans live with it today, while the UK counts approximately 5.8 million cases. Across Europe, estimates suggest over 60 million adults have diabetes, a figure that has climbed steadily as populations age and lifestyle patterns shift. The condition develops when the body either stops producing sufficient insulin or cannot use what it does produce effectively, sending blood glucose levels climbing dangerously high.
Here's where the research gets interesting. The relationship between sleep and metabolic health follows what scientists call an inverted U-shaped curve. Translation: more sleep improves insulin sensitivity up to a point. Beyond approximately 7.3 hours, however, additional sleep actually begins to harm it. This upends the common assumption that you can simply sleep your way to better health.
The weekend sleep trap nobody talks about
You might imagine that sleeping extra on weekends could make up for a week of short nights. The data suggests this approach is far more complicated than that simple fix. Researchers found that weekend catch-up sleep only helps if you've genuinely accumulated a sleep debt during the workweek. For those already getting adequate rest on weeknights, extending sleep on weekends may actually backfire and worsen metabolic health. This means your Sunday morning lie-in habit could be working against your body without you realizing it.
The underlying mechanism is particularly frustrating because it creates what researchers describe as a "potential vicious cycle." Metabolic dysfunction disrupts sleep quality, while high blood sugar can trigger the dawn phenomenon (waking too early) or frequent trips to the bathroom throughout the night. Poor sleep then compounds metabolic problems further, trapping people in a downward spiral that's genuinely hard to escape.
Sleep loss and appetite chaos
Part of sleep's impact on diabetes risk operates through appetite regulation. Naveed Sattar, a cardiometabolic medicine professor at the University of Glasgow, explains that poor sleep leads to weaker appetite control, causing people to eat more and make careless food choices. When you're exhausted, your judgment about what and how much to eat deteriorates significantly. Combined with metabolic dysfunction, this creates a perfect storm for weight gain and rising diabetes risk.
While a 2024 study did find that catching up on sleep reduced stroke and heart attack risk by roughly 19 percent, the relationship between rest and metabolic health remains genuinely complex. The researchers themselves caution that their work is observational and cannot definitively prove cause and effect. What it does suggest, though, is that sleep patterns should become a serious consideration for healthcare providers managing diabetes prevention.
Finding your sleep balance in the real world
Getting the right amount of sleep sounds simple in theory but becomes dauntingly difficult in practice. The wellness industry offers endless advice, from 8-6-4 breathing techniques and herbal teas to melatonin supplements and strict screen curfews. Yet actual human life rarely cooperates with perfect sleep hygiene protocols.
The next breakthrough may not emerge from another research study but from technology itself. Personalized apps combining real-time glucose monitoring with precision sleep tracking and sleep-enhancing audio could finally help travelers and busy professionals nail their personal optimal sleep window. Such tools already exist in various forms, and they're only becoming more sophisticated. For anyone managing diabetes risk while navigating irregular travel schedules or shift work, this convergence of data and technology might be worth exploring.