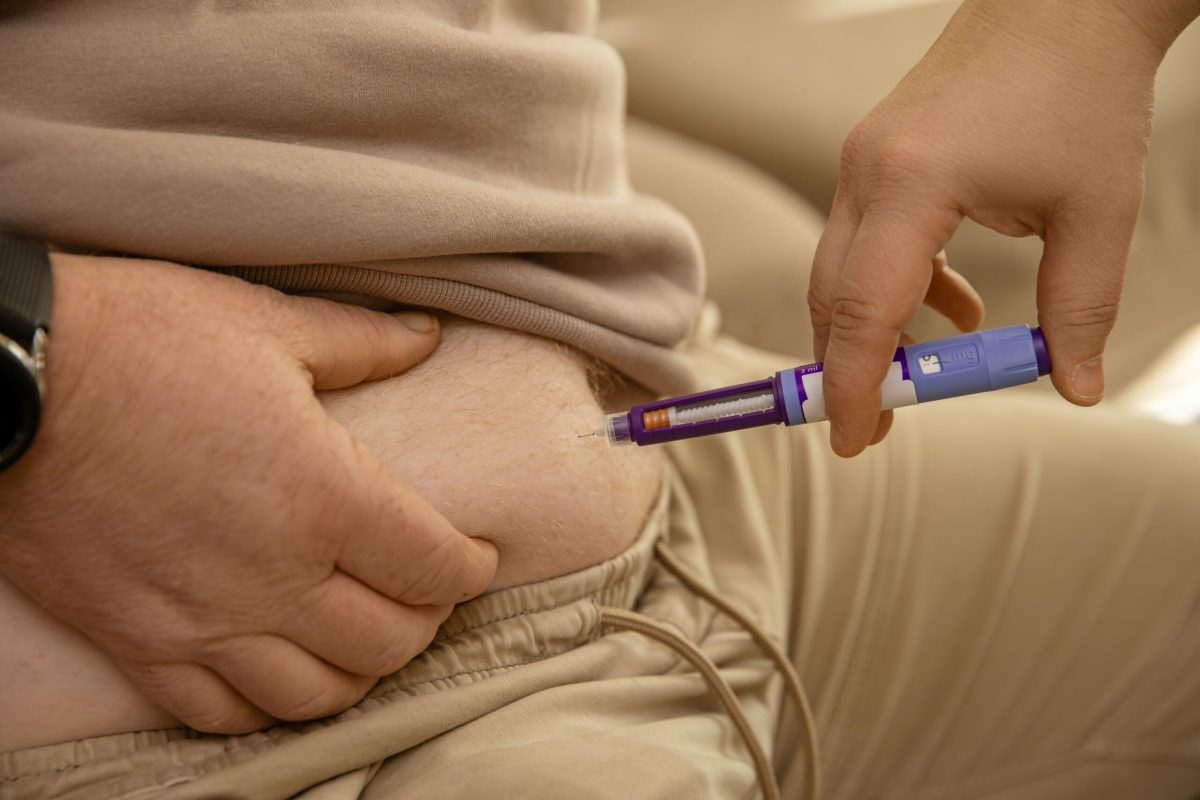
Here's a plot twist in modern medicine: the same drug your neighbor takes to lose weight might become a lifesaver for heart attack patients. A new study published in Nature Communications reveals that GLP-1 receptor agonists, already famous for treating type 2 diabetes and obesity, pack an unexpected superpower in cardiac care.
The culprit these drugs could defeat is something cardiologists call the "no-reflow" phenomenon, and it's far more sinister than it sounds. Even after emergency surgery clears the main artery during a heart attack, blood can't reach certain parts of the heart muscle. Roughly half of all heart attack patients experience this problem, and surgeons have essentially hit a wall trying to fix it. The blockage isn't in the big vessel anymore. It's in the microscopic capillaries that surgeons simply cannot access.
The Tiny Guardians That Won't Relax
Your heart's smallest blood vessels are wrapped in microscopic muscle cells called pericytes. During a heart attack, these cells clench like fists and refuse to let go. When they stay contracted, no amount of emergency surgery can force blood through. Svetlana Mastitskaya, lead author of the Bristol study, explains the stakes bluntly: "In nearly half of all heart attack patients, tiny blood vessels within the heart muscle remain narrowed, even after the main artery is cleared during emergency medical treatment."
The statistics are sobering. A 1% increase in vessel blockage predicts a 14% spike in deaths and an 11% jump in hospitalizations within a year. This isn't a minor complication. It's often the difference between walking out of the hospital and not.
Enter GLP-1. Your gut naturally produces this hormone as a messenger between your digestive system and your bloodstream. When researchers tested GLP-1 in lab conditions mimicking heart attacks, something remarkable happened. The drug essentially flipped a biological off-switch, signaling those stubborn pericytes to relax through special potassium channels in their cell membranes. Suddenly, the microvasculature reopened, blood flowed where it had been blocked, and heart damage diminished significantly.
A Drug with a Track Record
The clever part of this discovery is that GLP-1 drugs aren't experimental. Diabetic patients have been using them safely for years. Previous studies already showed fewer strokes and heart attacks among people taking these medications. What's new is the mechanism, the proof that they actively protect heart tissue during the most critical moments.
Doctors caution that using GLP-1 specifically as a weight loss drug remains relatively new, and long-term effects demand more scrutiny. But the safety profile from decades of diabetes treatment provides reassurance. The conversation around sustained use for cardiac protection may shift once these findings gain traction.
Pills Aren't Magic, But Neither Is Skipping the Gym
Before you start imagining a pharmaceutical cure-all, Harvard researchers have a reality check. A major study tracking heart health found that patients who stuck to eight lifestyle habits cut their risk of developing heart disease by approximately 60 percent. The habits include eating well, exercising regularly, not smoking, sleeping enough (but not excessively), drinking moderately, managing stress, maintaining strong social ties, and avoiding opioids.
Frank Hu, one of the Harvard study's authors, nailed the balance: "Even in the era of highly effective GLP-1 pharmacotherapy, lifestyle habits remain central to diabetes management and cardiovascular risk reduction, and can substantially amplify the benefits of modern medications." In other words, take the drug if it's prescribed to you, but don't treat it as permission to skip your morning run.
The real promise here isn't that science has solved heart disease. It's that doctors may soon have a tool that works at the microscopic level, reopening pathways that current surgery cannot reach. For heart attack survivors facing that dangerous no-reflow complication, that's not just progress. That's a second chance.